Energy for Health, Vol. 15, 2016
S.R. Olmos
President of the American Academy of Craniofacial Pain and Founder of the TMJ & Sleep Therapy Centres International
Abstract
Recent reports show that nearly half of adult Americans are living with chronic pain and one quarter are at high risk of obstructive sleep apnea (OSA), a sleep breathing disorder (SBD). The relationship between chronic pain and sleep is well documented. However, patients seeking treatment for pain symptoms have historically been treated independently from those seeking treatment for SBDs.
The purpose of this paper is to highlight the benefits of the MLS® laser system for the treatment of typical neuralgia of the lingual nerve and the comorbidity of chronic pain and sleep related breathing disorders.
A 66 year-old male was referred to our office for the relief of left mandibular episodic facial pain neuralgia. The patient had refractory treatment relief from two different anti-convulsant medications directed from different neurologists. The patient was screened in our office and referred to a Board Certified Sleep Physician and found positive for OSA (obstructive sleep apnea). The patient was treated with OAT (oral appliance therapy), MLS® laser and CPAP.
The patient had complete elimination of his chronic pain and discontinued his medications and continues to be free of pain two years later.
These results establish the efficacy of the MLS® laser in the treatment of neuropathy and in combination with the treatment of OSA and bruxism as a mechanism for nerve entrapment demonstrates a long-term cure.
Introduction
Classical trigeminal neuralgia (TN) is a disease of severe stabbing neuropathic facial pain of the second and third divisions of the trigeminal nerve [1]. It is estimated that 1 in 15,000 people suffers from trigeminal neuralgia; however, numbers may be significantly higher due to frequent misdiagnosis [2]. The incidence is greatest in people over 50 years of age and women more frequently than men [3].
It has also been reported that 26% of the American population were at high risk of obstructive sleep apnea (OSA), a sleep breathing disorder (SBD), indicating as many as one in four Americans could benefit from an evaluation for OSA [4]. In the same report, 57% of obese individuals were at high risk for OSA. Obesity is defined as a BMI (body mass index) of 30 or greater.
This case study seeks to demonstrate a longterm cure for trigeminal neuralgia utilizing lowlevel laser therapy and treatment for OSA. This case demonstrates relief of chronic facial pain of the mandibular division of the trigeminal nerve as it innervates the muscles of mastication (see Figure 1).
Trigeminal neuropathy can have many origins such as a neoplastic growth compressing the nerve as it leaves the pons and before it leaves the cranium through either the foramen rotundum (maxillary division, blue arrow) or foramen ovale (mandibular division, green arrrow), see Figure 2. Tumours, usually posterior fossa meningiomas or neuromas, are found in 2% of patients who present with typical TGN [5]. Surgical excision is indicated for these conditions as diagnosed via MRI.
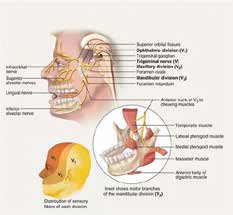
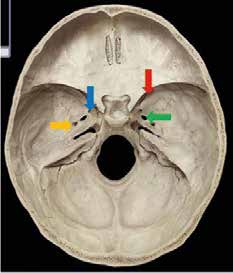
Another source of trigeminal neuralgia can be enlargement of the middle meningeal artery that can compress the mandibular division as it leaves the skull through the foramen ovale. The middle meningeal artery is a branch of the maxillary artery in the infratemporal fossa. It enters the skull through the foramen spinosum (yellow arrow Figure 2), and is within the dura mater lining the cranial cavity. The critical abnormality is vascular contact at the dorsal root entry zone, rather than more distally; such is seen in 3–12% of trigeminal nerves at autopsy [6,7]. Brain Surgery (microvascular decompression), is necessary to treat this condition.
The most common source of trigeminal neuralgia is peripheral entrapment of the nerve by the muscles it innervates or mechanical trauma (injury). There is damage to the myelin shealth that lowers the capacitance of the nerve that lowers its’ threshold for conduction. So there is a spontaneous transmission of pain in a sensory nerve by contractions of the muscles it innervates or a structure that it passes through. It has been my experience that mandibular trigeminal neuralgia is often present in combination with a movement disorder termed bruxism. Bruxism is an exacerbation of normal rhythmic masticatory muscle activity that results in wear of dentition and muscle pain disorders. The brain is stimulated by a variety of factors including pain, medications and sleep-related breathing disorders [8].
Treatment for trigeminal neuralgia is usually medicinal. Membrane stabilizing drugs, anti-convulsants, centrally acting muscle relaxants individually or in combination are used. Dosages are increased over time as tolerance, metabolism of the drugs increase and their effectiveness decreases. When maximum dosage for each individual drug has been reached it is lowered and an additional drug is combined until maximum dosage is reached and a third drug or new combination is tried. Commonly used drugs are Tegretol (carbamazepine), Neurontin (gabapentin), Lamictal (lamotrigine), Clonopin (clonazepam), Baclofen, (Lyrica (Pregabalin).
The clinical efficacy of low level laser therapy (LLLT) in the treatment of neuropathic pain is well established in many studies [9-19]. This is a very important tool for the treatment of nerve injuries as all other treatments are palliative while the laser therapy is truly therapeutic.
Case Study
A man 66 year-old was referred to our office for the relief of left mandibular episodic facial pain neuralgia by an oral maxillofacial surgeon. His chief complaints were chronic pain (four years) when chewing, jaw and facial pain. He had spontaneous shooting pain on the left side of his face. He said he could relate it to a novocaine injection and tooth implant. He was currently being treated with carbamazepine 100 mg four times daily, but the pain was not controlled. He had previously been treated with gabapentin 300 mg three times per day until it became ineffective. He sometimes took alcohol and sedatives for pain relief or sleeping.
Positive findings from his health history were high blood pressure, stroke, asthma, hepatitis, and frequent awakenings at night. Our clinical findings at time of examination were: BMI 31.07, B.P. 166/100, Pulse 64, Respirations 16, Temperature 98.2. Orthopedic mandibular ranges of motion were 56 mm without pain, left and right lateral movements of 10 mm, and 9 mm of protrusion. Dental examination demonstrated molar class one occlusion, with 4 mm of overjet and overbite, with worn dentition (bruxism), see Figure 3.
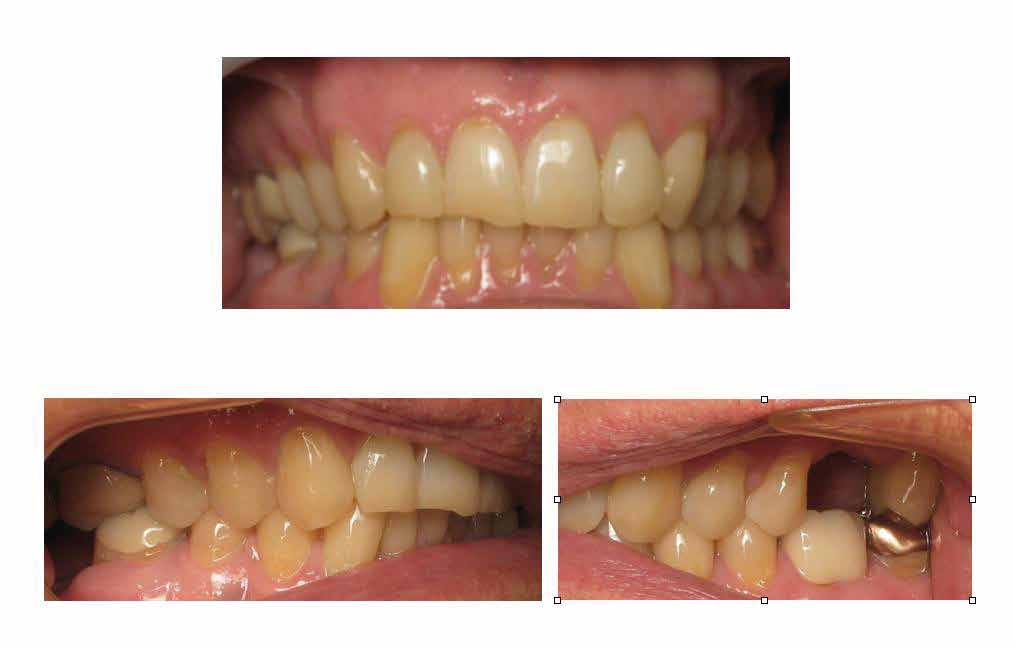
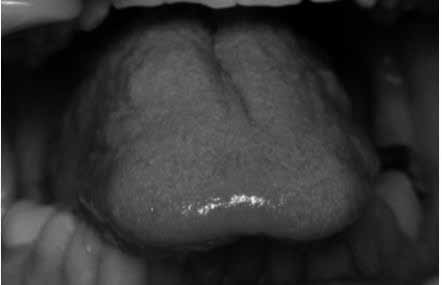
Oral evaluation demonstrated Mallampati class 4, furrowed tongue, coating of the tongue (indicating mouth breathing from nasal obstruction), and scalloping of the tongue, which are both indicative of a sleeprelated breathing disorder, see Figures 4 and 5.
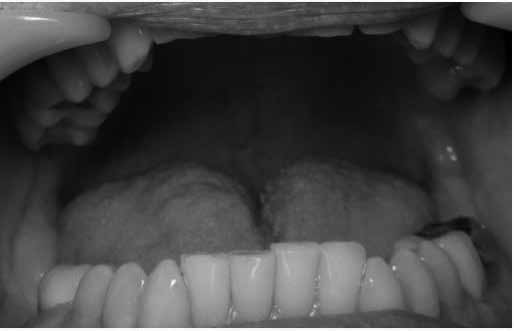
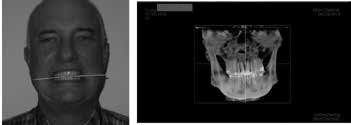
There were no positive findings for muscle, tendon and ligament palpation. Imaging utilizing CBCT (cone beam computed tomography) demonstrated a significant cant of the mandible to the left side (affected side) and was confirmed with photograph of patient with tongue blade, see Figures 6 and 7. This indicates that the elevator muscles or muscles of mastication are shorter on the left than right. When muscles are shorter than their resting length they have greater resting tonus or tension.
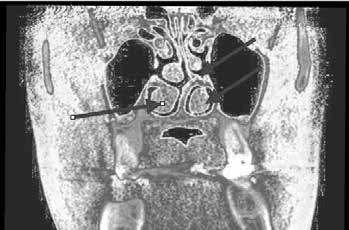
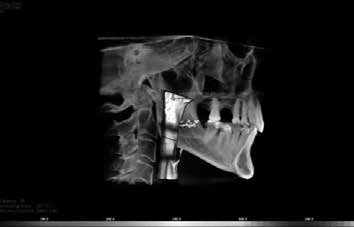
Nasal obstruction was observed from the iCAT CBCT, with deviation of the septum to the left with nasal soft tissue hypertrophy, see Figure 8. The oropharyngeal airway appeared to be within normal dimensions while awake, however it did not measure how much it can collapse while asleep, see Figure 9.
The diagnosis for this patient was trigeminal neuralgia with suspected sleep-related breathing disorder, nasal obstruction, nasal valve compromise, and bruxism. The treatment plan consisted of:
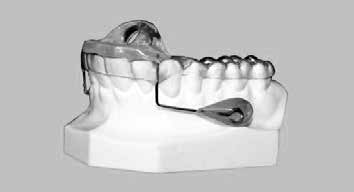
- Decompression appliance therapy, see Figure 10, (night orthotic that prevents mandibular retrusion, reduces clenching forces and opens nasal valve), for cant correction and leveling of the occlusal plane utilizing the phonetic or sibilant phoneme registration [20] and reducing of oropharyngeal airway collapse while sleeping with combined use of weekly treatments with a dual wavelength, high power IR laser (Multiwave Loked System (MLS®) laser, Mphi, ASA srl, Vicenza, Italy) see Figure 11, using the following treatment parameters: 50% intensity, frequency of 100 Hz, for 2-3 minutes utilizing energy of 30 joules and carbamazepine 100 mg four times per day. Treatment time 10-12 weeks and re-evaluation.
- Referral to sleep physician for diagnostic PSG (polysomnography).
- Referral to ENT physician for evaluation and treatment for nasal obstructions.
Treatment Results
At four weeks of the combined treatment of decompression, carbamazepine and weekly applications with the Mphi laser the facial pain and jaw pain had resolved and the pain when chewing had reduced between 40-50%. The unique synergistic use of two wavelengths of energy (808 and 905) using both pulsed and continuous (chopped) application is superior to either pulsed or continuous laser systems. The laser was used from the peripheral point of the innervation of the masseter nerve working back centrally towards its’ origin. Laser radiation can stimulate biochemical reactions and repair processes [21,22]. Since the damaged nerve has low threshold and is easily stimulated to transmit nociception/pain, it is necessary to keep the patient on medication to control the nerve while it is being healed. Once the nerve healing is complete and it retains its’ normal threshold or capacitance the need for medications is unnecessary.

At eight weeks of combined therapy and weekly applications of the Mphi laser the pain when chewing was resolved as well as the facial and jaw pain. At this point I recommended reduction of the carbamazepine dosage by one third and continued reduction until elimination of the drug or return of pain symptoms. The patient finally agreed to have a sleep study (PSG), and I wrote the prescription for referral.
At eleven weeks he had an attended sleep study (PSG) and the results were overall moderate apnea with and AHI of 26.0 and a REM AHI of 40.4 (severe). He had zero (0) stage 3 delta wave restorative sleep and his lowest oxygen desaturation was 82%. His periodic limb movement (PLM) index was 21.4. He was diagnosed with obstructive sleep apnea and PLM disorder.
At re-evaluation at 13 weeks of treatment the patient had completely weaned off all medications and was symptom free. He chose not treat his OSA and his PSG testing was performed without the decompression appliance. He found that he a slight tingling of the same injured nerve when he did not wear his oral decompression appliance for three nights. It was explained to the patient the severe health risks of untreated OSA.
This article demonstrates the relationship between trigeminal nerve injury and muscle contraction disorders such as those found in patients with sleep-related breathing disorders. Most importantly it demonstrates the value of laser therapy utilizing the unique delivery of the Mphi laser system on healing injured nerves. This is the most remarkable tool that I have seen in my 30 years of treating chronic pain disorders.
Bibliography
- Katusic S, Beard C.M, Bergstralh E, Kurland LT. Incidence and clinical features of trigeminal neuralgia, Rochester, Minnesota, 1945-1984. Ann Neurol.1991;27:89-95.
- Cheshire WPJ, Wharen REJ. Trigeminal neuralgia in a patient with spontaneous intracranial hypotension. Headache 2009;49:770–3.
- National Institute of Neurological Disorders and Stroke, National Institutes of Health, Bethesda, MD. www.ninds.nih.gov (trigeminal neuralgia)
- Hiestand DM, Britz P, Goldman M, Phillips B. Prevalence of symptoms and risk of sleep apnea in the US population: Results from the national sleep foundation sleep in America 2005 poll. Chest 2006 130 (3):780-786. doi:10.1378/chest.130.3.780
- Cheng TMW, Cascino TL, Onofrio BM. Comprehensive study of diagnosis and treatment of trigeminal neuralgia secondary to tumours. Neurology 1993; 43: 2298–302
- Hamlyn PJ, King TJ. Neurovascular compression in trigeminal neuralgia: a clinical and anatomical study. J Neurosurg 1992; 76: 948–52.
- Hardy DG, Rhoton AL Jr. Microsurgical relationships of the superior cerebellar artery and trigeminal nerve. J Neurosurg 1978; 49: 669–788
- Mayer P, Heinzer R, Lavigne G. Sleep Bruxism in Respiratory Medicine Practice. Chest 2016, 149(1):262-71.
- Iijima K, Shimoyama N, Shimoyama M, Yamamoto T, Shimizu T, Mizuguchi T. Effect of repeated irradiation of lowpower He-Ne laser in pain relief from postherpetic neuralgia. Clin J Pain. 1989;5:271–4.
- Walker J, Akhanjee L, Cooney M, Goldstein J, Tamayoshi S, Segal-Gidan F. Laser therapy for pain of trigeminal neuralgia. Clin J Pain. 1988;3:183–7.
- Iijima K, Shimoyama N, Shimoyama M, Mizuguchi T. Evaluation of analgesic effect of low-power He:Ne laser on postherpetic neuralgia using VAS and modified McGill pain questionnaire. J Clin Laser Med Surg. 1991;9:121–6.
- Walker J. Relief from chronic pain by low power laser irradiation. Neurosci Lett. 1983;43:339–44.
- Eckerdal A, Bastian H. Can low reactive level laser therapy be used in the treatment of neurogenic facial pain? A doubleblind, placebo controlled investigation of patients with trigeminal neuralgia. Laser Therapy. 1996;8:247–52.
- Moore KC, Hira N, Kramer PS, Jayakumar CS, Ohshiro T. Double blind crossover trial of low level laser therapy. Practica Pain Management 1988;1-7.
- Samosiuk IZ, Kozhanova AK, Samosiuk NI. Physiopuncture therapy of trigeminal neuralgia. Vopr Kurortol Fizioter Lech Fiz Kult 2000:29-32. [In Russian].
- Vernon LF. Low-level laser for trigeminal neuralgia. Practica Pain Management 2008:56-63.
- Kemmotsu O, Sato K, Furumido H, Harada K, Takigawa C, Kaseno S. et al. Efficacy of low reactive-level laser therapy for pain attenuation of postherpetic neuralgia. Laser Therapy. 1991;3:71–5.
- Kim HK, Jung JH, Kim CH, Kwon JY, Baik SW. The effect of lower level laser therapy on trigeminal neuralgia. Journal of the Korean Pain Society. 2003;16:37–41.
- Mann SS, Dewan SP, Kaur A, Kumar P, Dhawan AK. Role of laser therapy in post herpetic neuralgia. Indian J Dermatol Venereol Leprol. 1999;65:134–6.
- Singh D, Olmos S. Use of a sibilant phoneme registration protocol to prevent upper airway collapse in patients with TMD. Sleep Breath 2007.
- Mognato M, Squizzato F, Facchin F, Zaghetto L, Corti L. Cell growth modulation of human cells irradiated in vitro with low-level laser therapy. Photomedicine and Laser Surgery, 2004, 22(6): 523-526.
- Gigo-Benato D, Geuna S, De Castro Rodrigues A, Tos P, Fornaro M, Boux E, Battiston B, Giacobini-Robecchi MG. Low-power laser biostimulation enhances nerve repair after end-to-side neurorrhaphy: a double-blind randomized study in the rat median nerve model. Lasers Med Sci. 2004;19(1):57-65. Epub 2004 Jul 30.



