Energy for Health, Vol. 17, 2018
E. Perez, J.A. Natera, LD. Guzmán Hernández, J. Olalde
Centro Médico Adaptógeno, Calle Dr. Santiago Veve & Calle Marti #1, Bayamón, PR 00961, Estados Unidos
Cervical radiculopathy is the clinical description of pain and/or neurological symptoms resulting from any type of condition that irritates a nerve in the cervical spine (neck). Any condition that somehow compresses or irritates a cervical nerve can cause cervical radiculopathy.
Discogenic disease affecting the cervical spine is common cause of cervical radiculopathy and represents a disabling conditions which is caused by a damaged vertebral disc, particularly due to degenerative disc disease. Cervical radiculopathy caused by degenerative changes was first described by Parkinson in 1817 and still remains one of the major contributors for neck pain, commonly seen condition across many patient populations [1, 2].
Cervical radiculopathy symptoms typically include pain, weakness, or numbness in the areas served by the affected nerve. Pain can be felt in one area only, like the shoulder, or progress along the entire arm and into the hand and fingers.
The treatment involves nonsurgical (such as rest, physical therapy, manual manipulation, pain management with medications or injections) and surgical (anterior cervical discectomy and fusion and artificial disc replacement) treatments. Usually, if there is no improvement in symptoms after 6 to 12 weeks of treatment and nonsurgical treatments are not providing pain relief from cervical radiculopathy, or if neurological symptoms of arm or hand numbness and weakness continue to progress, surgery may be considered. Surgical intervention of the cervical spine can cause serious complications.
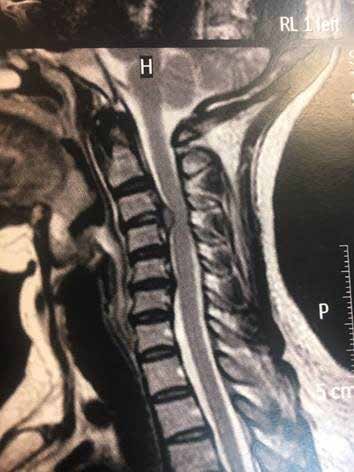
A woman 46 years old was referred to our study for the relief of pain associated to cervical radiculopathy. MRI of the neck showed signs of discogenic disease with disc desiccation at C2-C3, C4-C5 and C5-C6.
A slight loss of disc height was observed from C3-C4 to C5 (Figure 1). Presence of fluid, probably related to inflammation, was detected at the C3-C4 level, where a disc herniation was also shown. Disc herniation was located centrally and towards the right respect to midline, exerting a mass effect on the spinal cord, which was 50% narrowed. A small posterior disc protrusion was reported at the C5-C6 level, while in correspondence of C6-C7 level uncovertebral osteophytosis was present. Based on this radiographic data and on the clinical evaluation performed, the doctor proposed laser therapy to the patient in the attempt of proving pain relief and avoid cervical spine surgery.
The treatment plan included laser therapy in the cervical area and complementary botanical anti-inflammatory medicine, containing Rhodiola rosea, Morinda citrifolia, Tribulus terrestris, Uncaria tomentosa, Dioscorea villosa, Capsicum annuum.
The patient was treated with a dual wavelength, high power IR laser (Multiwave Locked System (MLS®) laser, M6, ASA srl, Vicenza, Italy), using the following treatment parameters:
- Handpiece: 50% intensity, frequency of 700 Hz, for 8 minutes utilizing energy of 9.5 Joules/cm2.
- Robotized head: 50% intensity, frequency of 700 Hz, for 8 minutes utilizing energy of 2.5 Joules/cm2.
Sensitive area trigger points were been identified and treated with handpiece, while robotized head was used to cover the overall treatment area.
Treatment was performed every day for 8 consecutive days.
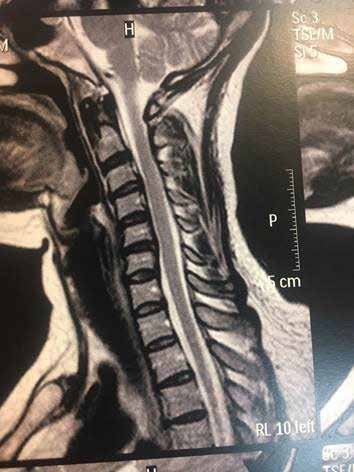
At the end of the treatment, the patient was pain free and, remarkably, MRI conducted to evaluate the patient 2 months after the first radiographic assessment (Figure 2) revealed that spontaneous regression of the herniated disc had occurred, with 90% restitution of the spinal cord space.
In the reported case, not only MLS® therapy provided an effective non-invasive approach to treat cervical pain, but the remarkable result observed in this case is the successful outcome on the spinal cord narrowing. It is important to note that there have been fewer reports of spontaneous regression of cervical disc herniation, especially ones confirmed by magnetic resonance imaging [3, 4]. Many factors related to the regression process have been recognized, including the age of the patient, dehydration of the expanded nucleus pulposus, resorption of a hematoma, revascularization, penetration of herniated cervical disc fragments through the posterior longitudinal ligament (PLL), the size of disc herniation, and the existence of cartilage and annulus fibrous tissue in the herniated material. Resorption of a herniated nucleus pulposus is thought to occur via an inflammatory reaction in the outermost layer of the herniation, with macrophages as the major cellular population [5]. It can be hypothesized that MLS® therapy could be a useful method to facilitate the mentioned factors.
In conclusion, the main result for the patient was elimination of pain and avoidance of surgical intervention, which in our experience is the most common outcome of this type of cervical condition.Bibliography
- Evans G. Identifying and Treating the Causes of Neck Pain. Medical Clinics of North America. 2014;98(3):645–661.
- Cervical radiculopathy: a common cause of neck pain. American Family Physician. 2016;93(9).
- Mochida K., Komori H., Okawa A., Muneta T., Haro H., Shinomiya K. Regression of cervical disc herniation observed on magnetic resonance images. Spine. 1998;23(9):990–995.
- Kobayashi N., Asamoto S., Doi H., Ikeda Y., Matusmoto K. Spontaneous regression of herniated cervical disc. Spine J. 2003;3(2):171–173. Regression of cervical radiculopathy after laser therapy treatment – a case report. Energy for Health [17]
- Pan H, Xiao LW, Hu QF. Spontaneous regression of herniated cervical disc fragments and its clinical significance. Orthop-Surg. 2010;2(1):77-9.